 Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. Not too long ago on a rainy Saturday, my kids were pacing around the house, bored trying to figure out something to do together since they couldn’t go outside to play. They were restless with energy to burn. Then one of them suggested the game hide and seek to the squealing delight of my 3 year old because she loves that game. The countdown began and the sound of scurrying feet reverberated around the house as each child rushed to find the best possible hiding spot. For a few moments, there was actually silence in my house while the search began, which was refreshing. But then you could start to hear little giggles and chuckles as each child was found in their hiding spots and eventually a new round started. As the game wore on and more rounds were played, the excitement of finding their siblings grew and grew to the point that in the last few rounds, there was raucous squealing and laughter of pure delight every single time one sibling was found. In the midst of all the noise and happiness of a classic game on a rainy day, I found myself reflecting on the situation I was observing. It reminded me so much of what Jesus tells us in his word speaking to Zaccheus. “And Jesus said to him, ‘Today salvation has come to this house, since he also is a son of Abraham.’ For the Son of Man came to seek and to save the lost.” Luke 19:9-10 Much in the same way my kids were out searching for each other with joy and anticipation, we too, as followers of Christ with a disciple-making command should follow in Jesus’ footsteps and seek out the lost with joy and anticipation. We come into contact with so many people during the course of our day. Family members. Colleagues. Co-workers. Patients. And the list goes on. I needed that reminder from my kids. And maybe you need that reminder too - that we are to be seekers of the lost in order to bring them to Jesus and salvation. But the other part of watching a rainy day Hide and Seek game unfold in my home was the utter excitement, joy, and laughter when one was found. It reminded me again of God’s word when Jesus is teaching his disciples. “I tell you, there will be more joy in heaven over one sinner who repents than over ninety-nine righteous persons who need no repentance.” Luke 15:7 “Just so, I tell you, there is joy before the angels before the angels of God over one sinner who repents.” Luke 15:10 It is incredible to me that God could have used any means to bring lost souls to himself but He, in His wisdom, ordained me and you to seek those who are lost, those who need to be found and brought to the light. And what a joy it is when salvation is granted. What a cool thought that we get a role in making all of heaven rejoice! So, who will you seek out in these days to bring to the father? Jason ***Check out my book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***
0 Comments
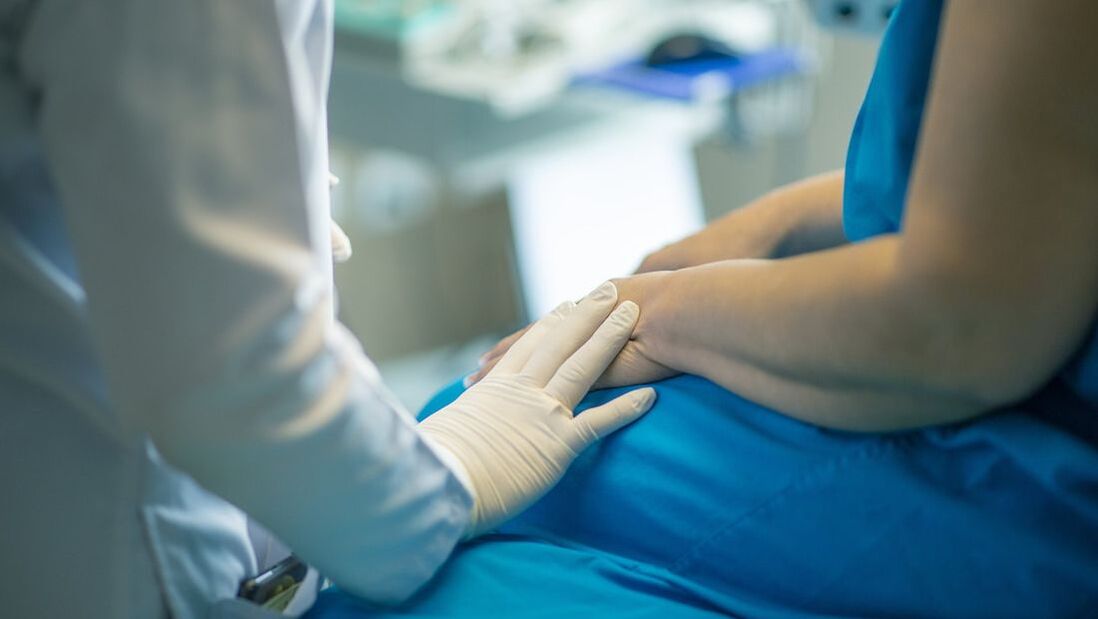 Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. I am beyond thrilled today to have another friend and colleague back on the blog today in our "Faith at Work" series. Please welcome Megan Mobley to the discussion! She has graciously put together some thoughts and encouragements for us from her perspective of working as a PT in a burn unit. And if you want to get caught up with the series you can view previous therapists thoughts on these links: Neuro Rehab, Spinal Cord, Management, Ortho/Sports Rehab, Acute Care 1, Acute Care 2. Enjoy! Where do you work? Describe the patient population in which you work. Since graduating in 2010, I have been working as a PT at the regional burn center in Augusta, GA (Joseph M. Still Burn Center), which happens to be the largest in the USA. All of my patients have impaired skin, whether it be burn injuries or complicated wounds (necrotizing fasciitis, Stevens-Johnson syndrome, pyoderma gangrenosum, calciphylaxis). I am also involved in wound care in our outpatient clinic that involves scar management after burn injury, smaller non-healed burns, or less complicated wounds (venous, arterial, diabetic, pressure). What do you enjoy about working in that field of PT? Never did I expect to go into wound care, but I have always loved the hospital setting. The burn center is such a special place. No one expects to get injured, and families are uprooted from around the southeast portion of our country (we have some international patients too), in order to come to Augusta, GA for treatment. I am able to walk along the patient and their family members during the most traumatic event of their lives. What are some of the unique physical, emotional, or spiritual challenges of working in that field PT? I touched on some of this above, but burns are an unexpected trauma. A loved one is recovering in the hospital, who may have been the breadwinner of the family, a father of 3 kids, and lives in a town 3 hours away from Augusta. Families take turns visiting. Some patients have no visitors. Many staff members are burned out from working in this setting, and treat it only as a job. It has to be so much more than that! Patients are in the hospital from just a few days to 6-12 months prior to their first admission home. Some patients never make it out of the hospital unfortunately. It can take a toll on you emotionally, but you have to stay focused on the long term of getting that patient as independent as possible and returning home. Your co-workers are a great support system. We work very closely together and support one another. In this setting, your co-workers truly are the only ones who understand your day. Patients are always in pain, but they are able to receive some pain medications, but therapy is never pain free here. I love educating the patient and their family on what their new normal may look like upon discharge home. How does your faith impact your work and how you view your patient interactions? Loving others above myself. Loving my patients and their family members even when they are unlovable. I can extend this love because Jesus first loved me. I try to be compassionate and put myself in the patient's or caregivers' shoes because this is their first experience going through a catastrophic burn injury (even though I have seen it countless times). I try to explain and educate them on healing timelines and what to expect during recovery. It is not an easy place to work, but I see it as a mission field. We have patients who tried to commit suicide but were given a second chance. I try to point those things out that the patient has a purpose and is still here for a reason. Briefly describe a story in which you really felt like you ministered to a patient and their family. There was a young couple that I worked with several years ago, and the woman was injured over 50% of her body including the most visual areas of the body: her face and hands. Her husband was at her side every day in the hospital, and their home was 3 hours away. He would participate in our therapy sessions, and he was always so engaged saying “She is my best friend. I will do anything for her.” It is a full time job for a caregiver when a patient with a large burn injury discharges home: lotion application and massage every 2 hours, donning compression garments and wearing them 23 hours/day, stretching, exercises. I was able to be there for this patient and her husband as they transitioned home after being in the hospital for several months with a burn injury that was not fully healed. I tried to educate and give them home exercise programs and other resources to help them prepare for managing everything at home. This particular couple ministered to me as well because their love and commitment were so strong to one another! Over the years, I have seen other spouses leave their partners after this type of injury because “this wasn’t the life I signed up for.” Megan ***Check out my book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. Hello Everyone! Thank you for your patience with this blog. I mentioned a few months ago that my wife and I were having another baby girl and I was going to take pause. Well, now she is 3 moths old and we are enjoying having a little snuggly one in our house. I am finally feeling like I can get back to this platform a little bit, albeit slowly. So, I am excited to be back! And since I've been off for a little while, I thought I'd post a Journal Club from one of recent work discussions. There are always many fun topics and research to discuss when talking about ACL rehab, recovery, and return to sport. We’ve even talked about some of the new research and ideas when it comes to ACL rehab on this platform. But one of the interesting aspects that often gets pushed to the back burner if you will is the psychology of return to sport after ACL injury and recovery. In a previous Journal Club on this blog, we looked at a recent study involving the importance of looking at confidence and return to sport and provided an additional tool for you to use in your clinic to consider the mental state of your patient in reference to their rehab process and readiness to return to sport. Similarly, a recent study came out looking at self reported fear and ACL recovery - specifically fear of activity after ACL and re-injury and this was the topic of our most recent residency journal club meeting. ACL Reconstruction and Self-Reported Fear The researchers found 40 patients who were cleared for return to sport and had them fill out the Tampa Scale of Kinesiophobia (TSK-11) along with other standard functional measures. Then these patients were tracked over a 12 month period to identify any subsequent ACL injury. The results were interesting and lend credence to what we might have assumed. Essentially, the researchers found that, indeed, a higher score on the TSK-11 showed decreased activity levels of the year and increased risk of re-injury. So, much like the functional measure we discussed previously on confidence, this study also validates the usage of a fear based outcome measure to help us better identify at risk patients for re-injury. We can subsequently use that information to help educate and tailor strength interventions to decrease the TSK score and improve that patient's activity level and ultimately quality of life. Jason ***Check out my book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. I want to first of all thank all of you for the feedback over the past few years. It is encouraging to hear from y’all about the impact this blog and platform has had since its inception. It truly warms my heart and helps me to continue to write and build content. I really do love writing and publishing helpful content both here and postings on other social media platforms. But sometimes life situations change and a pause is required in something you love doing to preserve the family/marriage/life/work balance. So, in order to prevent myself from getting overextended , I have an announcement to make. I will be taking a few months off from writing and publishing blog content. Not because I am out of ideas or because I’ve lost interest but because of an exciting life event coming up: My wife and I will be having another baby girl in the next few weeks!! We are thrilled to bring another child into our family but that will necessitate more dedicated time to my family for the time being. I will still continue to try to post brief quotes, verses, and other articles on the facebook page @ptsonmission. So you can continue to follow over there to stay connected. I will also use this time to try to move current content onto different platforms like YouTube. And this will be a great time to hear from y’all too, so don’t hesitate to post or message me! Thank you for understanding and if you are enjoying this platform please continue to share and spread the word. I will be back with y’all in a few months! Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. I do love the Christmas season. It can often become overwhelming with traveling, family gatherings, parties, and shopping but even in the midst of all the festivities and activities it is still an exciting time because there are those parties and gatherings with friends and family, and Christmas lights, and cookie decorating, and caroling and hot chocolate and nostalgic music. It is, indeed, a special time. It’s a uniquely special time for me, too, because I celebrate my wedding anniversary five days before Christmas so there is an added romantic feel every year for me. My kids have also made my Christmas seasons extra joyful because of their daily excitement and longing for Christmas morning as they dream about the gifts they will receive and the reaction of those you will receive gifts from them. But most importantly, in the midst of the holiday season, is the intentional reminder of the good news of great joy that we celebrate: Christ’s coming. The fulfillment of God’s great redemptive plan finally coming to fruition. The reality that peace with God will finally be made possible through the forgiveness of sins. Christmas is such a precious and treasured time. And to help remind us of that great rescue plan, we often sing! I love the music of Christmas and one of my favorite hymns to sing every year is “Angels from the Realms of Glory." Embedded in the lyrics is the complete story and picture of redemption. So, I just want to leave the lyrics here for you as you celebrate Christmas this season to remind you of this good news of great joy. Angels from the realms of glory, Wing your flight o’er all the earth; Ye who sang creation’s story Now proclaim Messiah’s birth. Shepherds, in the field abiding, Watching o’er your flocks by night, God with us is now residing; Yonder shines the infant light: Sages, leave your contemplations, Brighter visions beam afar; Seek the great Desire of nations; Ye have seen His natal star. Saints, before the altar bending, Watching long in hope and fear; Suddenly the Lord, descending, In His temple shall appear. Sinners, wrung with true repentance, Doomed for guilt to endless pains, Justice now revokes the sentence, Mercy calls you; break your chains. Though an Infant now we view Him, He shall fill His Father’s throne, Gather all the nations to Him; Every knee shall then bow down: All creation, join in praising God, the Father, Spirit, Son, Evermore your voices raising To th’eternal Three in One. Come and worship, come and worship, Worship Christ, the newborn King. Have a wonderful holiday season and Merry Christmas!
Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. I recently ran across a fascinating article in the most recent edition of the Journal of Orthopedic and Sport Physical Therapy (JOSPT). If you are not familiar this this journal, it is a popular publication in the outpatient sports and orthopedic physical therapy world. They cover a wide range of topics from unique sport case studies to intervention control trials to literature reviews. So what was the unique article? It was about the need to begin to research and study the impact of mechanics and musculoskeletal injury in, none other than, E-Sports. That's right. Gaming. It is certainly an unconventional topic but as I began to read through the article it provided many fascinating statistics and legitimate arguments for exploring this largely unstudied arena of sport - if we classify gaming as a sport. More Than a Game Article In the article, the authors discuss some of the mind blowing statistics around esports including the billions of dollars of revenue and millions of viewers for esport events. It really is fascinating. They then go on to detail that this may be an untapped patient population for physical therapists because of growing musculoskeletal injury reports related to repetitive movements and static postural changes. The authors highlight that there is not much research but that maybe we should begin to explore this field further because it could really impact our profession. So it got me thinking about you in your clinic. Have you seen patients who participate in esports in your practice? Is this a trend you have noticed in your clinic and, if so, have you identified any patterns of esport injury? I hope you get a chance to peruse through this article just because it is interesting and my be somewhat prophetic in the trends of sport. Who knew that esport would begin to compete with traditional sport and require the skill of physical therapists! Jason  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. As we approach the holiday season with Thanksgiving kicking things off, I thought it would be nice to reflect on an attitude of thankfulness. I recently read this poem that really spoke to me. I hope it encourages you and helps you set the tone as we all pause from the daily grind of our busy lives and just give thanks. "Heavenly Father, on Thanksgiving Day We bow our hearts to You and pray. We give You thanks for all You've done Especially for the gift of Jesus, Your Son. For beauty in nature, Your glory we see For joy and health, friends and family, For daily provision, Your mercy, and care These are the blessings You graciously share. So today we offer this response of praise With a promise to follow You all of our days." -Mary Fairchild Have a wonderful Thanksgiving with all of your family and friends from PT's on Mission!! Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. I’m sure you are familiar with the old adage sticks and stones may break my bones but words will never hurt me. Cute, for sure, but wildly inaccurate. If we are honest with ourselves we have all been hurt by words. That’s why it’s no surprise that the Bible includes so much instruction on how we use our tongue. God wants to remind us that our words have meaning, power and can either build up or tear down. I mean, just look at what James says regarding our tongue and the words that come out of it. “For every kind of beast and bird, of reptile and sea creature, can be tamed and has been tamed by mankind, but no human being can tame the tongue. It is a restless evil, full of deadly poison. With it we bless our Lord and Father, and with it we curse people who are made in the likeness of God.” James 3:7-9 That's some strong language! Bottom line is our tongue and the words we say can bring life or bring destruction and we want to make sure that we are bringing life because we can’t take back the damage our words may cause. I remember a powerful analogy that helped me solidify this principle and I have done this same analogy with my kids. I gave them a small tube of toothpaste and told them that the toothpaste inside is your words. Then I told them to squeeze out all the toothpaste on the plate. They had a blast squirting the toothpaste everywhere. Then I told them to try and put the toothpaste back in the tube. Guess what? It couldn’t be done and so the lesson was watch what you say because you can’t undo what you say. You can’t put the toothpaste back in the tube. You can try but once it’s out, it’s out. Hopefully that analogy helps you a little bit as we are reflecting on what we say and the weight of our tongue. I have not mastered this. I am a work in progress on this topic and that is partly why I’m writing this because I know I’m not alone and recently I have learned some helpful tips, which I will share in just a minute. But first, what does this have to do with physical therapy? Two quick points: What we say to our patients and colleagues matters. We want to make sure that we are kind in our speech to our patients. We don’t always know what a patient may be going through in their life. We don’t always understand what may be occurring behind the scenes. So we must guard what we say and make sure that we are encouraging and building them up. Same with our colleagues. We should speak in a manner that edifies them and does not tear them down. What we say about our patients and colleagues matters. There is probably nothing worse than being torn down in secret behind your back. And I have been so convicted in my life and practice in this regard. It is so easy after a patient encounter that might have been weird or awkward or frustrating to sit down with our colleagues and vent or poke fun at the patient or patient interaction. Brothers and sisters, this ought not to be so. I am the first to admit that I have failed in this regard and that is part of the conviction to write this blog. We want to speak life about a patient even if they are not right in front of us. And if we can’t speak in a worthy manner about someone, then maybe we just need to hold our tongue. Again, we don’t know what the patient may be going through but we must remember that they are still created in God’s image and worthy of dignity. Now, sometimes patients or colleagues do some funny things and it may be OK to share that story as long as the dignity and integrity of the person can be maintained. But I do think we need to be more careful with how we speak and what we say about patients in the office. So is there a way to help us remember to pause before we speak? Yes! This acronym from my Pastor is one that I have found to be very helpful in framing what I say and how I say it both in the workplace with my patients and colleagues and in my home. The acronym is T.H.I.N.K. I have attached a bunch of passages for you to look up and be reminded of how often the Bible speaks to our speech. Take the time and go through this acronym. T. Is it True - Prov. 15:2, 15:7, 15:28, 18:8 H. Is it Harmful - Prov. 12:18, 13:3, 29:11 I. Is it Inspiring - Prov. 10:21, 12:25, Eph 4:29 N. Is it Necessary - Prov. 10:19, 18:6-7 K. Is it Kind - Matt. 7:12 So next time when you are about to say something at your home with your family, at your workplace with your colleagues, or in a treatment room with a patient, T.H.I.N.K. before you speak and watch the words you say impact the people you interact with in a helpful, encouraging, and edifying way. Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. “An ounce of prevention is worth a pound of cure.” We have probably heard that old adage at some point in our lives. And the main principle behind it is that if you take care of the small things then you can often avert larger problems or issues. Think about your vehicle. I bet you take the time to make sure the fluids are good and that the oil is changed. You perform small, cheaper routine maintenance which will extend the life of the engine. You could ignore those things but as they pile up eventually the engine will fail and you have a much larger, more expensive issue. I think the same is true in the world of healthcare and especially physical therapy. The appropriate use of physical therapy for a number of musculoskeletal issues is a cost effective way to manage your health and prevent larger more expensive problems from occurring. Today’s article is yet another valuable piece of research that sheds light on the cost effectiveness of physical therapy. This study is about 6 years old but continues to be relevant as it is corroborated by many more recent studies. This article looks at back pain in particular and overall medical costs associated with and without physical therapy. This is certainly an article to save, digest, and use to educate your patients. Implications of Early Physical Therapy The bottom line of this article to me is when the researchers say, “Early and adherent physical therapy was associated with significantly lower utilization of advanced imaging, lumbar spinal injections, lumbar spine surgery, and use of opioids. Given the enormous burden of excessive and unnecessary care for patients with LBP on society, cost savings from early guideline adherent physical therapy has important implications of single payer health care systems to design optimal care process models for LBP.” In other words, for low back pain in particular, going to PT early and consistently significantly reduces the individual and societal health care cost. Another fascinating finding in the study was that not only was the musculoskeletal care cost lower but attending PT also had an effect in decreasing other in-patient healthcare costs. In other words, like we mentioned earlier, an ounce of prevention is worth a pound of cure. As people went through rehab, the primary problem was resolved but secondary issues improved as well because of exercise and movement. Cool stuff! I hope you utilize this study and others like it to help your patients understand the importance of physical therapy and what you are trying to do to help them. There are significant, wide-ranging effects from attending PT for low back pain and beyond. Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!***  Welcome to our new subscribers!! And if you haven't joined the conversation on Facebook, then find us @ptsonmission to continue to receive updates, encouragement, and information. Finally, tell a friend if you are benefiting from this site. In life it is often tempting to think far ahead into the future about things that we could be doing or about goals we want to achieve. Thinking long-term is not inherently a bad thing and we should consider planning for the future and having goals to achieve. But, I’ve been thinking recently about what is near, close, and those things that are not in the distance but right in front of me. We are comfortable working hard for distant things but we should be equally comfortable working hard on the tasks and relationships that are right in front of us. Much of this thought comes from a passage I recently read in the book of Ecclesiastes. Solomon is providing his reflection on life and what ultimately matters versus what is meaningless. Then, in chapter 9 he says this: “Whatever your hand finds to do, do it with all your might, for there is no work or thought or knowledge or wisdom in Sheol, to which you are going.” Ecc. 9:10 There are people, tasks, and opportunities all around us in which we can work hard with all our might to serve and make an impact. One of my faith heroes, C.H. Spurgeon sums this up well in his sermon on this passage when he says: “Here we will observe, first, that this refers us to the works that are near at hand. You are not called upon to-day, the most of you, to do works which your eye sees far away in Hindostan or China. The most of you are called especially to do the work which is near at hand. People are always desiring to be doing something miles off. If they could but be somewhere else what wonders they would accomplish! Many a young man thinks if he could stand up under a banyan tree, and discourse to the black faces in India, how eloquent he might be. My dear fellow, why don't you try the streets of London first, and see whether you are eloquent there. Many a lady imagines that if she could move in a high circle she would no doubt become another Lady Huntingdon, and do wonders. But why cannot you do wonders in the circle in which God has placed you? He does not call you to do that which is leagues away, and which is beyond your power; it is that which your hand findeth to do. I am persuaded that our home duties, —the duties which come near to us in our own streets, in our own lanes and alleys, —are the duties in which we ought most of us mainly to glorify Christ. Why will you be stretching out your hands to that which you cannot reach? Do that which is near, —which is at your hand.” Think about your life. Think about where you work. I think you will be able to begin to identify so many areas in which you can work with all your might. There are so many tangible things to do that are near. Now, this is not to neglect those distant things in which you may be called but it is to say, especially in this post-COVID environment to pray and search out the close opportunities. What might some of these things be? This is not an exhaustive list but here are four categories I’ve been thinking about. Work Hard in your Relationship with God. This may seem obvious but it is certainly something that is near at hand and something that we should work at with all our might. We should want to commune with God more, study his word more, know him more and more. As we do that we will begin to become more holy and more Christ-like. And truthfully, in our fallen nature, our tendency is to become complacent and lazy. There are times when it is easy to commune with God but there are also times when we have to work so consider that this is a glorious task at your fingertips. Work Hard in your Marriage and Family. I think we all understand for those of us that are married and have children that cultivating those relationships are incredibly important. The health of our marriages and our families speak volumes to a lost and hopeless world. We want to work hard to be a great spouse and parent. And to do so might require assessing our work/life balance and taking some time to rest like we talked about last week. Work Hard Investing in your Colleagues and Patients. We spend so much time with our co-workers and our patients that there are sure to be areas of ministry right in front of us. Our patients and colleagues are experiencing the ebb and flow of life’s hardships just as we do and we have an incredible opportunity right in front of us to minister and share God’s love and reconciliation. And if you are wondering about practical tips to minister to patients and co-workers then I would encourage you to pick up a copy of Rehab the World. Work Hard in your Community. I think it is important to be involved in the community in which you live by serving in different capacities to make a difference. I am reminded of the Lord’s admonition through Jeremiah to the Israelites when they were in captivity, in this regard. The Lord tells them to build homes, plant gardens and eat the produce and then to build families. Then the Lord commands the Isrealites to “seek the welfare of the city where I have sent you into exile, and pray to the LORD on its behalf, for in its welfare you will find your welfare.” Jer. 29:7 The community in which we live is certainly near at hand and we will benefit from seeking it’s welfare. Why does all this matter? Why should we work diligently in the work that is near at hand? Solomon gives the answer. It is because our days are fleeting. Our time is running out as each of us is one day closer to our death. And when that time comes, we will no longer have the opportunity to work with all of our might. Listen again to Spurgeon: “Let us pause a moment, and think that in a short time we must die. The hour is not to be staved off. I may preach to you to-day and exhort you to flee from the wrath to come; but when this tongue is sealed in silence, I can no more warn you. Mother, you can pray for your children, now; but when death shall have sealed your eyes in darkness, there can be no more prayers lifted up for ever. You may now, O Sunday school teacher, instruct those children, and God blessing you, you may be their spiritual father and bring them to Christ; but it shall one day be whispered in your class, "teacher is dead;" and there is the end of your labor. When once death shall have come you cannot devise liberal things; your brain cannot form new devices for the spread of your Master's kingdom, neither can your heart, then, bend and weep over sinners perishing, or your tongue address them with earnest exhortation. Think, dear friends, that all we can do for our fellows we must do, now.” I write this as a reflection and a challenge in my own life; obviously not wishing quick death on anyone, nor dwelling on death to the point of obsession, but I think we need to be reminded that we are not guaranteed tomorrow in order to be more effective believers today. So, let’s work with all our might in what is near at hand with a sense of hopeful urgency. Jason ***Check out the new book "Rehab the World" written for Physical Therapists to encourage us in our workplace and prepare us to serve those around us. If you like, please leave a review and spread the word!!*** |
Awesome ResourcesThe Gospel at Work Archives
April 2024
Categories |
 RSS Feed
RSS Feed